 One important problem is that normal ECG teaching does not include the following key points:ġ) Many obvious STEMI(+) LAD OMIs do not have any reciprocal ST depressions.Ģ) Many LAD OMIs cause STE and hyperacute T waves in the inferior leads, which is usually attributed to apical LV involvement registering in the inferior leads. Absence of ST elevation in ECG leads V7, V8, V9 in ischaemia of non-occlusive aetiologies. Poh K-K, Chia B-L, Tan H-C, Yeo T-C, Lim Y-T. showed that diffuse STD of subendocardial ischemia results in STD of all walls therefore, it stands to reason that the diffuse STE of pericarditis (if the pericarditis/myocarditis is diffuse and not localized, as it usually is) would result in diffuse STE of all walls. If a patient had acute STE in V1-V6, I, aVL, II/III/aVF, and V7-9, then I suppose it could truly be described as diffuse, since it is present in all major LV walls. Thus, it is not possible to determine whether a finding is diffuse on a standard 12-lead ECG, because we do not have posterior leads. Moreover, the standard 12-lead does NOT record posterior leads. In fact, there is reciprocal ST depression in aVL! Bischof and Smith showed that this does not happen in pericarditis, and happens nearly universally in inferior OMI. On this standard 12-lead ECG, there is Absence of diffuse ST elevation. "ĭiffuse implies that the finding is present in all walls of the LV, meaning it must include at least all of the following areas of the LV: anterior, lateral, posterior, and inferior. Look how the computer lists the criteria that led it to diagnose pericarditis: "ST >0.10 mV, ant/lat/inf." The computer, like most providers with average ECG education, is literally programmed to say that any ECG finding present in the anterior, lateral, and inferior leads is " diffuse. And for this reason, "you diagnose pericarditis at your peril." Three providers disagreed and unanimously agreed that there was "no reciprocal findings", and one of them agreed with the computer's interpretation seen here:įirst, and most important: anterior, lateral, and inferior ST Elevation is still far more likely to be OMI than pericarditis. (Or it might be too far away and with too much interposed lung to register any reciprocal STD) Posterior leads, if obtained, are likely to show reciprocal STD. The OMI findings are not at all diffuse, rather focal exactly to the areas listed above. 
The most common, important, and treatable etiology would of course be OMI until proven otherwise by emergent angiogram. This is diagnostic of acute transmural infarction of anterior, lateral, and apical LV areas. There is a small amount of reciprocal STD in aVL (reciprocal from lead III), as well as a reciprocally negative T wave which is inappropriate for that QRS. The T waves in V5 and V6 could also be increased in size and area compared to baseline, but no baseline was available. Hyperacute T waves are present in V2-V4, and II, III, and aVF. We see STE in V2-V4, and a hint of STE in II, III, and aVF.  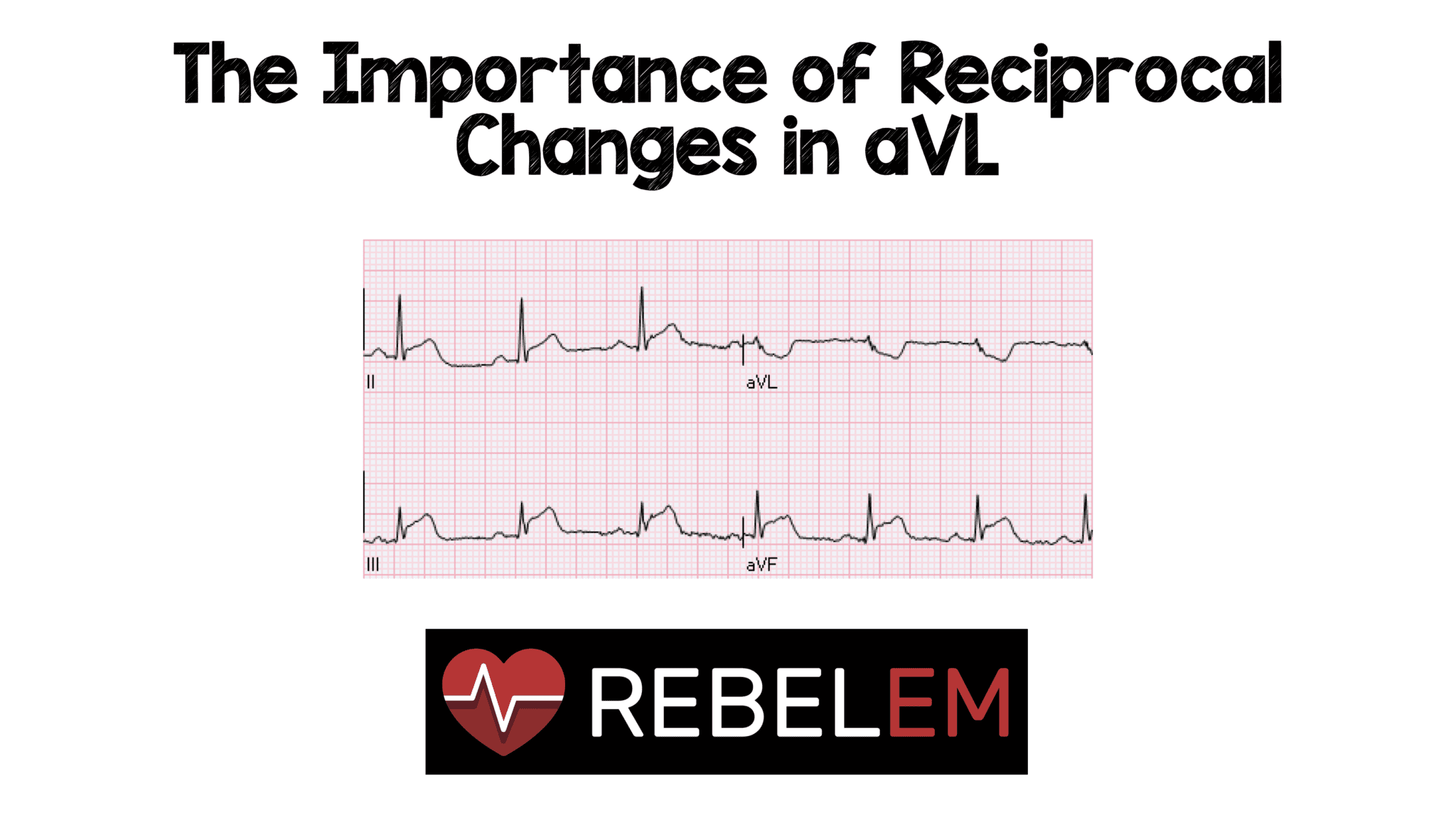
There is sinus rhythm with normal QRS complex except slightly sluggish R wave progression (this is due to acute LAD OMI, diminishing the R wave voltage in its distribution). We activated the cath lab because this is diagnostic of LAD OMI. EMS called in while I was on shift and asked me to review an ECG of a man in his 50s with acute chest pain and dyspnea that started approximately 45 minutes prior to arrival. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
